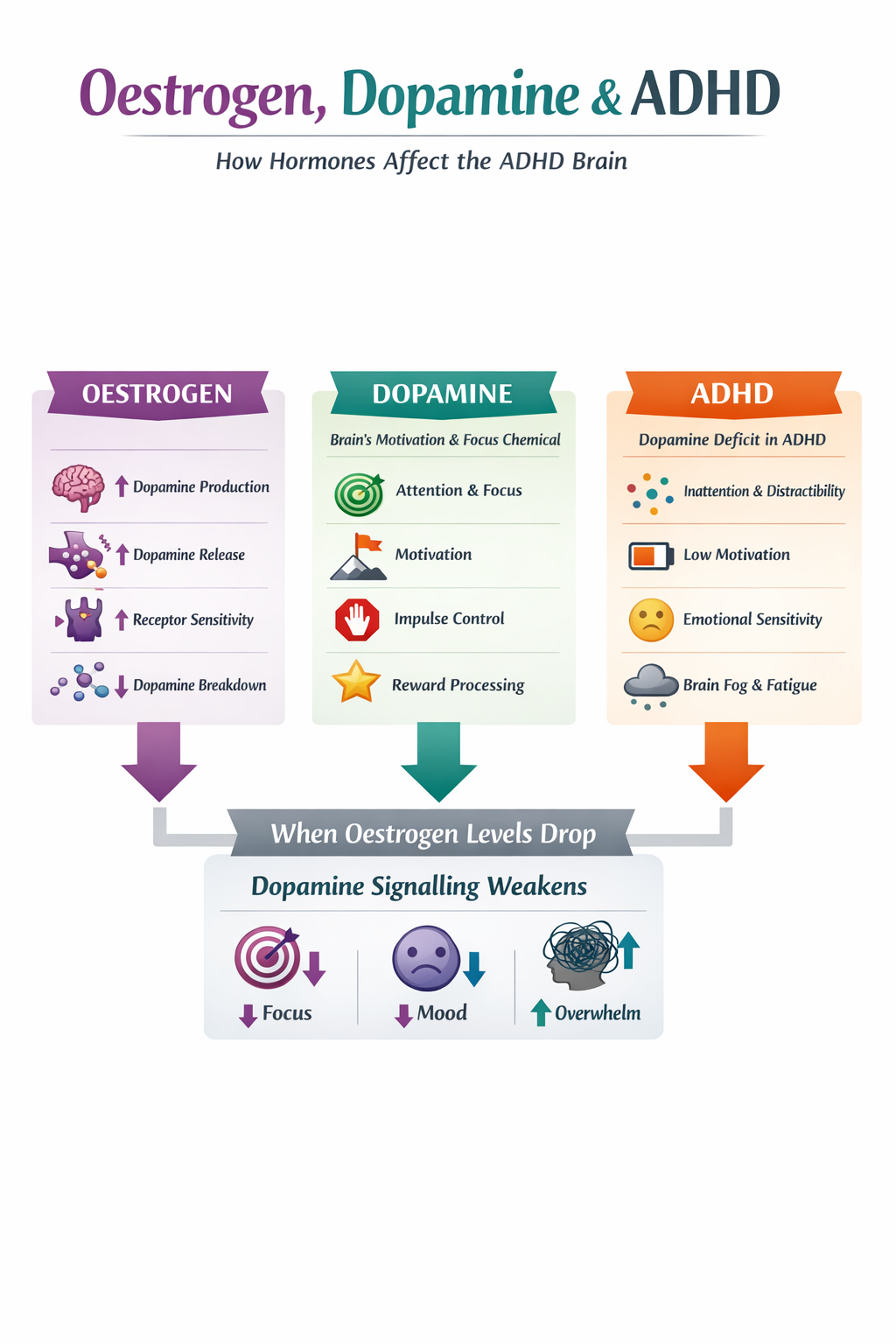
ADHD, DOPAMINE and OESTROGEN
Why many women notice changes in focus across the month and across life
For many years ADHD was viewed primarily as a condition affecting boys. We now know that this was more a reflection of how ADHD presents rather than who experiences it. It also has to do with the historical lack of research specifically focused on women (men are easier subjects because they don’t experience so many fluctuations!!)
Many women have spent decades managing the challenges of attention, organisation and overwhelm without recognising the underlying pattern. What often brings it into sharper focus is a change in hormones, and happily, we are now much more open to discussing the challenges women experience.
Often, women first start asking questions about ADHD during perimenopause, when concentration becomes harder, mental fatigue increases and familiar strategies seem to stop working. There may be changes in mood and an increase in anxiety, and frequently, feelings of being ‘stuck’ and unable to move forward.
The reason lies partly in the relationship between oestrogen and dopamine.
Dopamine and the ADHD brain
Dopamine is one of the brain’s key signalling chemicals. It plays a central role in the networks that allow us to prioritise, act and stay engaged with tasks.
In practical terms dopamine helps with:
• sustained attention - focus
• motivation
• task initiation - getting started (especially big tasks)
• working memory - remembering lists, enjoying reading
• impulse regulation
• emotional balance
Brain imaging studies show that ADHD is associated with differences in dopamine signalling in areas such as the prefrontal cortex and striatum, both of which are important for planning, decision making and regulating behaviour.
This is why stimulant medications often help people with ADHD. They increase dopamine availability in these brain systems, helping things feel more manageable.
Where oestrogen comes in
Oestrogen does far more than regulate reproductive biology, which is where we tend to hear about it most. It also interacts with many neurotransmitter systems in the brain. One of the most important interactions is with dopamine.
Research shows that oestrogen can:
• increase dopamine synthesis so that we have enough of it
• increase dopamine release
• enhance dopamine receptor sensitivity, meaning that it’s more available when we need it
• reduce dopamine breakdown
In simple terms, oestrogen supports the brain’s dopamine system. When oestrogen levels are higher, dopamine signalling tends to be more efficient. When oestrogen levels fall, dopamine activity may decrease.
For women with ADHD, whose dopamine systems already work a little differently, these hormonal shifts can make symptoms even more noticeable.
Research in neuroscience and women’s mental health shows that oestrogen modulates dopamine activity in the brain, influencing attention, motivation and executive function. Fluctuations in oestrogen are associated with changes in ADHD symptoms across the menstrual cycle and during perimenopause (Kooij et al., 2025; Osianlis et al., 2025; Eng et al., 2024).
Monthly changes
Many women (with and without ADHD) notice predictable changes in focus across the menstrual cycle. During the late luteal phase -the days leading up to a period - oestrogen levels fall sharply.
At this point women often report:
• reduced concentration
• increased mental fatigue
• greater emotional sensitivity
• feeling more easily overwhelmed
• ADHD medication feeling less effective
These changes are not a lack of effort or discipline, they reflect the biological interaction between hormones and neurotransmitters.
Perimenopause and ADHD
Perimenopause is another time when this relationship becomes particularly visible. During this stage oestrogen levels fluctuate unpredictably and gradually decline.
Because oestrogen supports dopamine signalling, these fluctuations can affect the brain systems that support attention and mental organisation.
Women often describe:
• struggling to focus in meetings
• forgetting words or appointments
• feeling mentally scattered
• needing far more effort to stay organised
For some women this is the first time ADHD becomes clearly identifiable. It’s also when women come to see me for help. I often see women who say they don’t recognise themselves. They’ve lost their confidence and can’t see the way ahead. It’s not my role to diagnose ADHD. My role as a Solution Focused Hypnotherapist is to help people to find the best way to manage their experience.
A broader view of support
Understanding this biology can be reassuring. It explains why focus and mental clarity sometimes change across the month or across life stages. It also highlights the importance of supporting the brain in multiple ways.
In my HYPNOURISH© approach, I look at several foundations that help steady and manage brain function:
Sleep
The dopamine system relies heavily on restorative sleep. Even small improvements in sleep quality can support attention and emotional regulation.
Nutrition
Stable blood sugar and adequate fibre and protein intake support neurotransmitter production. Omega-3 fats and polyphenol-rich foods also support brain health.
Positive Action
Engaging in meaningful or enjoyable activity stimulates dopamine release naturally.
Positive Interaction
Supportive social connection reduces stress chemistry and improves cognitive resilience.
Positive Thought
Learning to guide attention intentionally reduces unnecessary threat signalling from the amygdala and allows the prefrontal cortex to work more effectively.
None of these strategies replace medical treatment when it is needed, but they form the foundations of long term mental wellbeing.
A useful shift in perspective
When women understand the relationship between oestrogen and dopamine, many experiences that once felt confusing begin to make sense. Changes in focus or motivation are not signs of personal failure, they are part of a complex interaction between hormones and brain chemistry. Once we understand that relationship, we can work with the brain more intelligently and with far more compassion for ourselves.
My information for this article has come from courses of study with -
Dr Sarah McKay - the Neuroscience Academy, In Her Head, the Neuroscience of the Female Brain
Dr Emily Prpa - The Nutrition Reporter and Seed Talks Gut Brain Connection
Dr Anneka Tomlinson - Seed Talks ADHD and Women
With reference to research cited in the article.